
Understanding
the Novel Coronavirus
COVID-19
last update 31 March 2020
What is COVID-19?
The 2019 Novel Coronavirus, also known as SARS-CoV-2, caused an outbreak of respiratory illness called COVID-19, in Wuhan, China. It has since spread to other parts of China and the world. Coronaviruses are a family of viruses that infect birds and mammals (this includes humans!). Typically, they cause mild respiratory symptoms similar to the common cold, but can lead to death, often in those that are already immunocompromised.
Quick look : How does COVID-19 compare to the other coronaviruses?
SARS
2002
In 8 mo
8,000
confirmed cases
9.6%
death rate
MERS
2012
In 36 mo
2,484
confirmed cases
34.4%
death rate
COVID-19
2019–Present
So far in 76 mo
704M
confirmed cases
1.0%
death rate
Live update of COVID-19 numbers
How deadly is COVID-19?19,20
While COVID-19 is much more infectious, it appears to be less deadly than SARS or MERS right now. However, it is more deadly than the annual flu, which has a death rate of less than 1%. This is why it is even more important that if you experience mild symptoms, you should seek medical care right away, and practice hygienic habits to slow the spread of germs and COVID-19 to the people around you.
China's COVID-19 death rate by age as of 11 Feb 202019,20

Note: Diseases do not have a single case fatality rate; it depends on context, and changes with time and location.
The first few months of COVID-1918
1 Dec 2019
First patient confirmed in Wuhan, China
31 Dec 2019
China sends urgent notice to WHO of unknown respiratory illness cause
7 Jan 2020
- New virus identified as a coronavirus
- Europe's first case confirmed in France
11 Jan 2020
First death is announced in China
21 Jan 2020
First case in the US is confirmed; Snohomish County, Washington
24 Jan 2020
First case of human-to-human transmission is confirmed outside of China in Vietnam
30 Jan 2020
- WHO declares the outbreak a global public-health emergency (PHE)
- The US reports the first confirmed instance of person-to-person spread
31 Jan 2020
- HHS Secretary declares a PHE for the US
- President Trump enforces a 14-day quarantine preceding the entry of travelers from mainland China into the US
11 Feb 2020
WHO announces a new official name for the disease as “COVID-19”
25 Feb 2020
CDC warns community to prepare for the spread of COVID-19 in the US
29 Feb 2020
First death in the US in King County, Washington
1 Mar 2020
UN releases $15 million USD from the Central Emergency Response Fund (CERF) to fund global efforts to contain the virus
11 Mar 2020
WHO announces that the COVID-19 outbreak is a global pandemic
13 Mar 2020
President Trummp declares a National Emergency, allowing those in charge to act faster in response to an emergency
What happens now?
COVID-19 has spread from Asia to North America, South America, Europe, Oceania, and Africa. The world continues to work towards treating the sick and containing the disease as we learn more about it. For now, the public is encouraged to practice social distancing and hygienic practices.
How is it spreading?6
At this time, we don't know how fast or easily this virus is spreading between people. More information is discovered everyday, but here's what we know so far.
Human-to-human transmission is possible
The virus first came from an animal source, but it is now able to spread from human to human.
It travels through droplets in the air
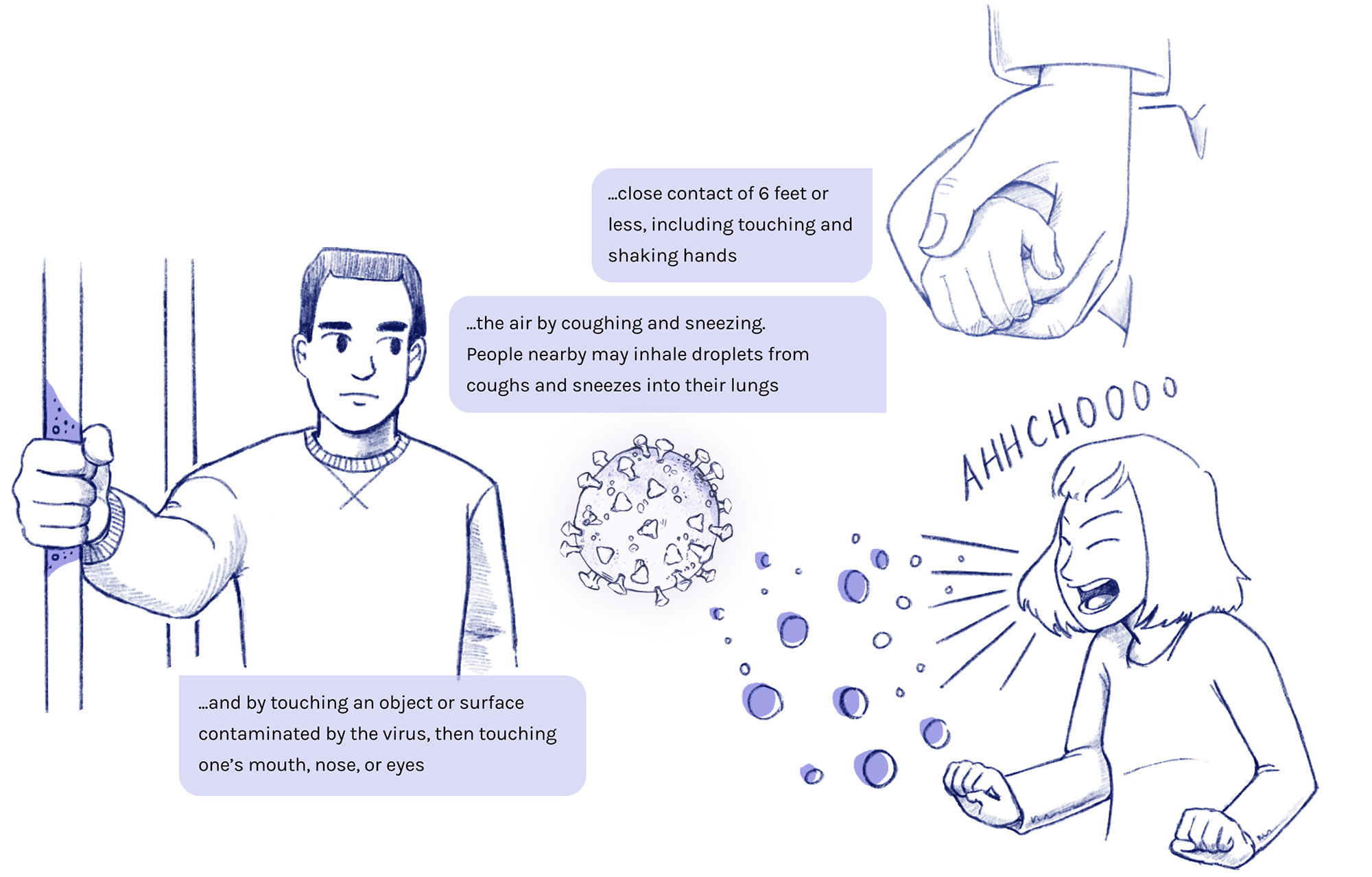
It can infect humans through...

...close contact of 6 feet or less, including touching and shaking hands.

...the air by coughing and sneezing. People nearby may inhale droplets from coughs and sneezes into their lungs.

...and by touching an object or surface contaminated by the virus, then touching one's mouth, nose, or eyes.
Incubation Period9
The time between exposure to the virus and the start of symptoms is between 5.2 - 12.5 days.

Your Part
Outbreaks at this scale can be scary, but besides staying up to date on the news, there are still a lot of things that you can do to stay healthy and help stop the spread of disease!
Prevention4
Here's what you can do to prevent COVID-19 from spreading to others:

Stay home when you are sick.
Wash your hands often with soap and warm water. If unable to wash your hands, use alcohol-based hand sanitizer.
Avoid close contact with people who are sick.
Clean and disinfect frequently touched objects and surfaces.
Cover coughs and sneezes with your elbow or a tissue. Throw tissues in the trash.
Get your annual flu vaccine.
Take flu antivirals if prescribed.
Avoid touching your eyes, nose, and mouth with unwashed hands.
Check CDC's COVID-19 travel health notices often and avoid nonessential travel.

Close Contact3
If you come into close contact with someone who is confirmed to have COVID-19,
here's what you can do to stay well:
- Monitor your health for at least 14 days after your last contact with the infected person.
- Watch for these signs and symptoms.
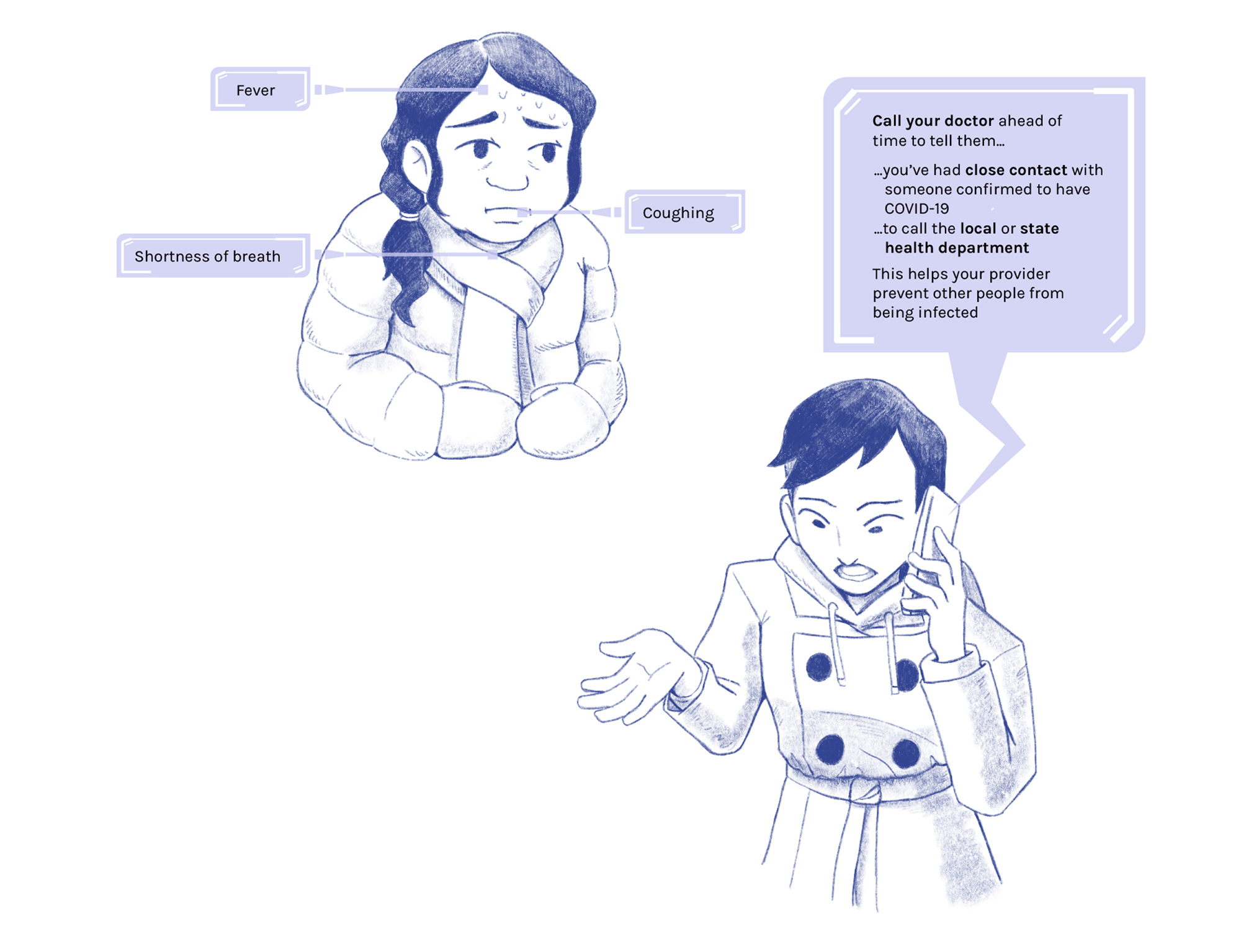
Contact your healthcare provider right away if you notice these signs:

Fever
Coughing
Shortness of breath
If you have any of these symptoms, call your doctor ahead of time to tell them...
...you've had close contact with someone with the COVID-19 infection
...to call the local or state health department
This helps your provider prevent other people from being infected.
Stay Calm, Take Care
Remember, don't panic!
Take care of yourself just like you would during the annual flu season.
Stay on top of the news and other credible sources to keep updated on if you need to do anything different.
Caring for Patients5
If you or someone you know becomes sick with COVID-19 and does not require hospitalization or is told they are medically stable to go home, here's what you can do to take care and prevent further spread of the disease for patients (P) and for caregivers (C).
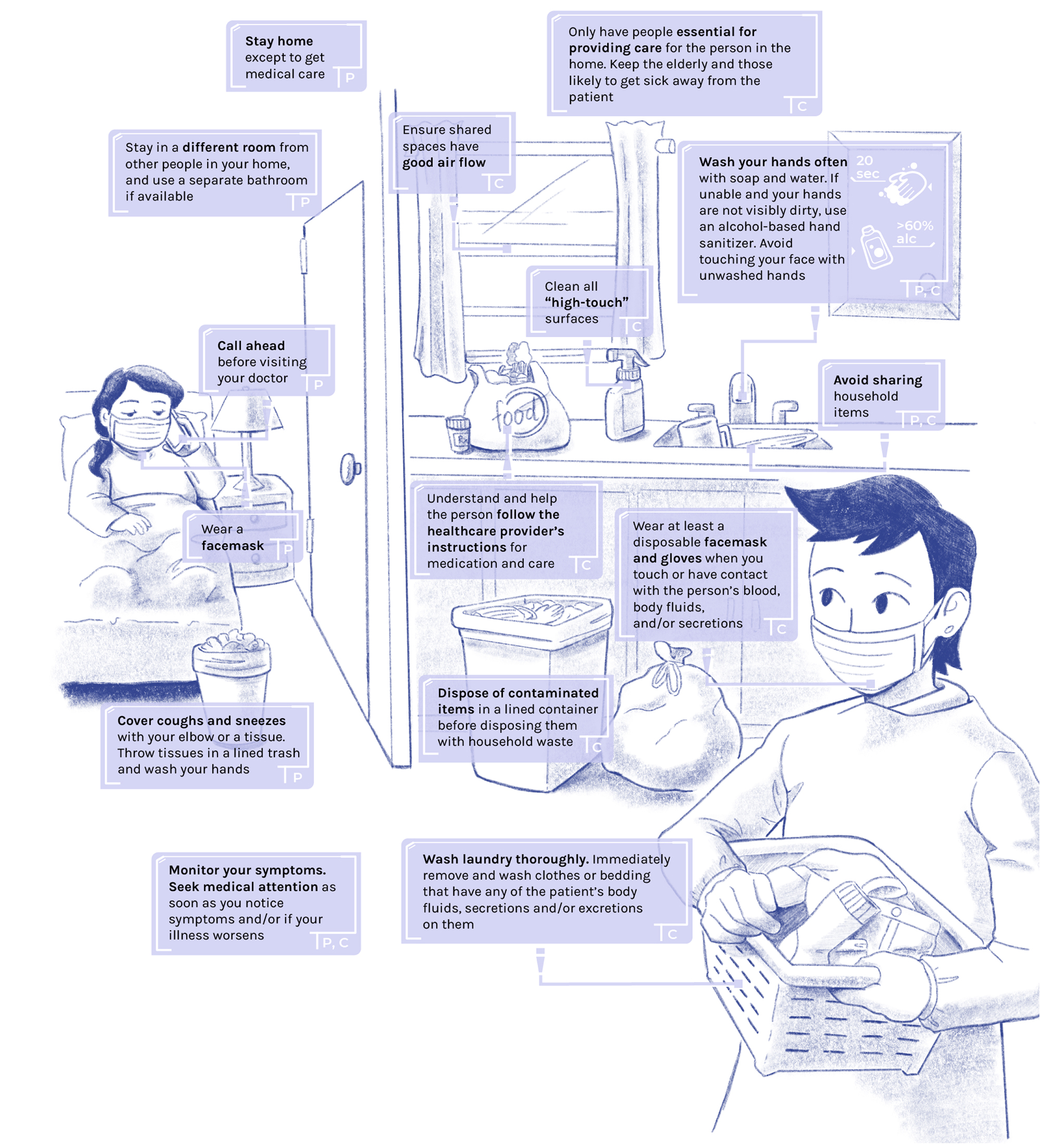
For Patients
Stay home except to get medical care.
Stay in a different room from other people in your home and use a separate bathroom, if available.
Call ahead before visiting your doctor.
Wear a facemask.
Cover coughs and sneezes with your elbow or a tissue. Throw tissues in the trash and then wash your hands.
Follow these precautions until you are fully recovered from COVID-19, to prevent the spread of disease and ensure you get better!
For Caregivers

Ensure shared spaces have good air flow.
Only have people essential for providing care for the person in the home. Keep the elderly and those likely to get sick away from the patient.
Clean all "high touch" surfaces.
Understand and help the person follow the healthcare provider's instructions for medication and care.
Dispose of contaminated items in a lined container before disposing them with other household waste.
Wear at least a disposable facemask and gloves when you touch or have contact with the person's blood, body fluids, and/or secretions.
Wash laundry thoroughly. Immediately remove and wash clothes or bedding that have any body fluids and/or secretions or excretions on them.
For Both Patients and Caregivers
Wash your hands often with soap and water for 20 seconds. If unable to and your hands are not visibly dirty, use an alcohol-based hand sanitizer (>60% alcohol). Avoid touching your face with unwashed hands.
Avoid sharing household items.
Monitor your symptoms, and seek medical attention as soon as possible if you notice any symptoms and/or if your illness worsens.
Healthcare providers and state/local health departments must be consulted to get permission to end home isolation. They will give their permission when the patient's risk of spreading COVID-19 to others is low; the timing differs from patient to patient.
Contact your state or local health department if you still have any questions.
Stay home and follow these precautions until you are fully recovered from COVID-19, to prevent the spread of disease and ensure that you get better!
Healthcare providers and state/local health departments must be consulted to get permission to end home isolation. They will give their permission when the patient's risk of spreading COVID-19 to others is low; the timing differs from patient-to-patient.
Contact your state or local health department if you still have any questions.
End the prejudice!4
Asian people are not at a higher risk than other people from becoming sick with COVID-19.
Only people who have traveled to high-risk areas or been in contact with someone confirmed or suspected to have COVID-19 in the last 14 days are at a higher risk of being infected.
Just because someone is of Asian descent does not mean that they have COVID-19!
Hospitals desperately need masks
Save the masks for those who need them most!1
In light of the outbreak, two kinds of facemasks have been flying off American shelves:
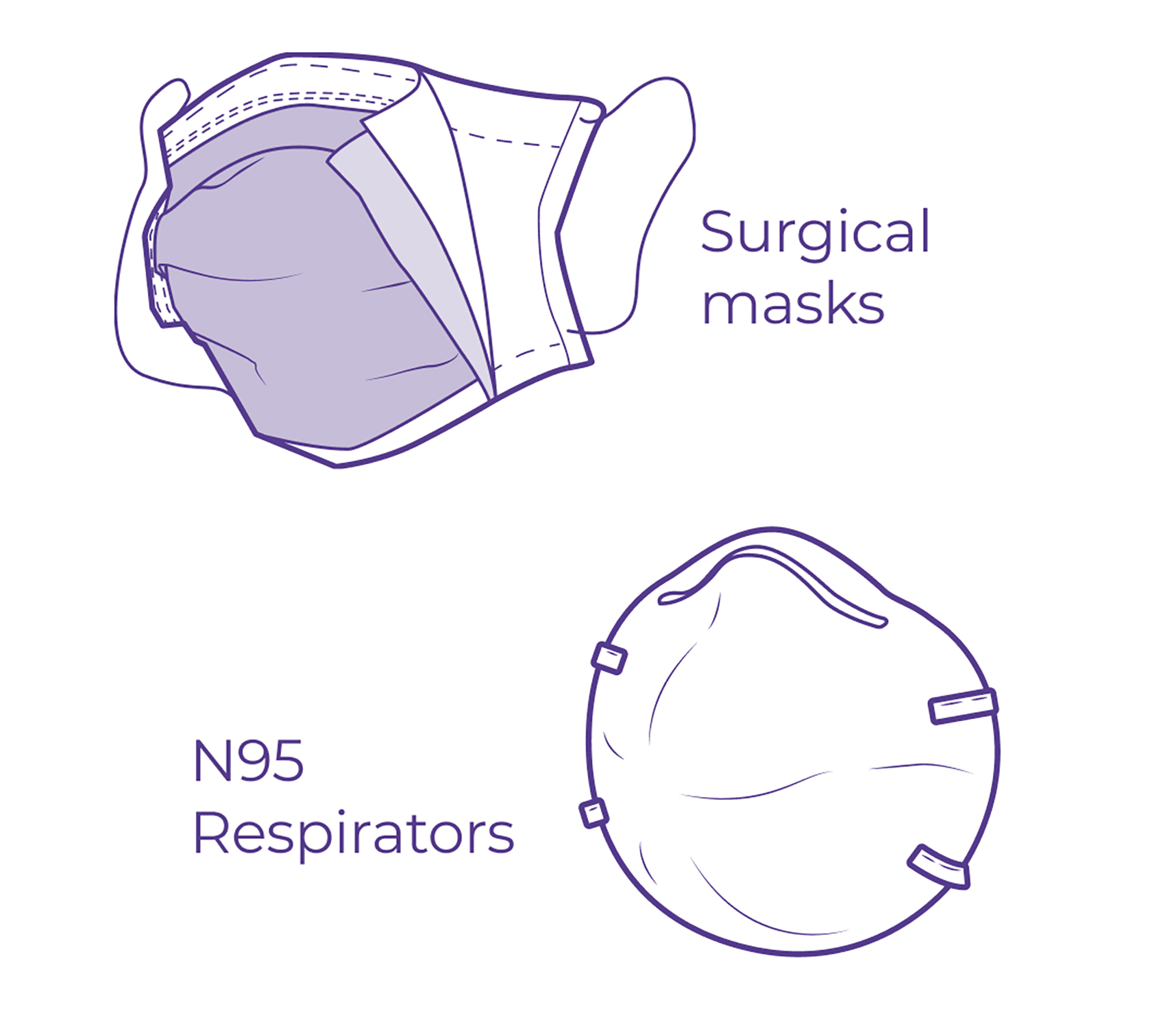
Surgical masks filter the wearer's sprays from sneezes and mucus from coughs, which will help prevent the spread of COVID-19 if you are sick, but does not effectively prevent catching COVID-19.
N95 respirators filter out at least 95% of small airborne particles. These will help prevent against catching and spreading COVID-19, but if it has a breathing valve, it does not effectively prevent the spread of COVID-19 if you are sick.
Surgical Masks

Will help prevent the spread of COVID-19 if you are sick
Does not effectively prevent catching COVID-19
N95 Respirators
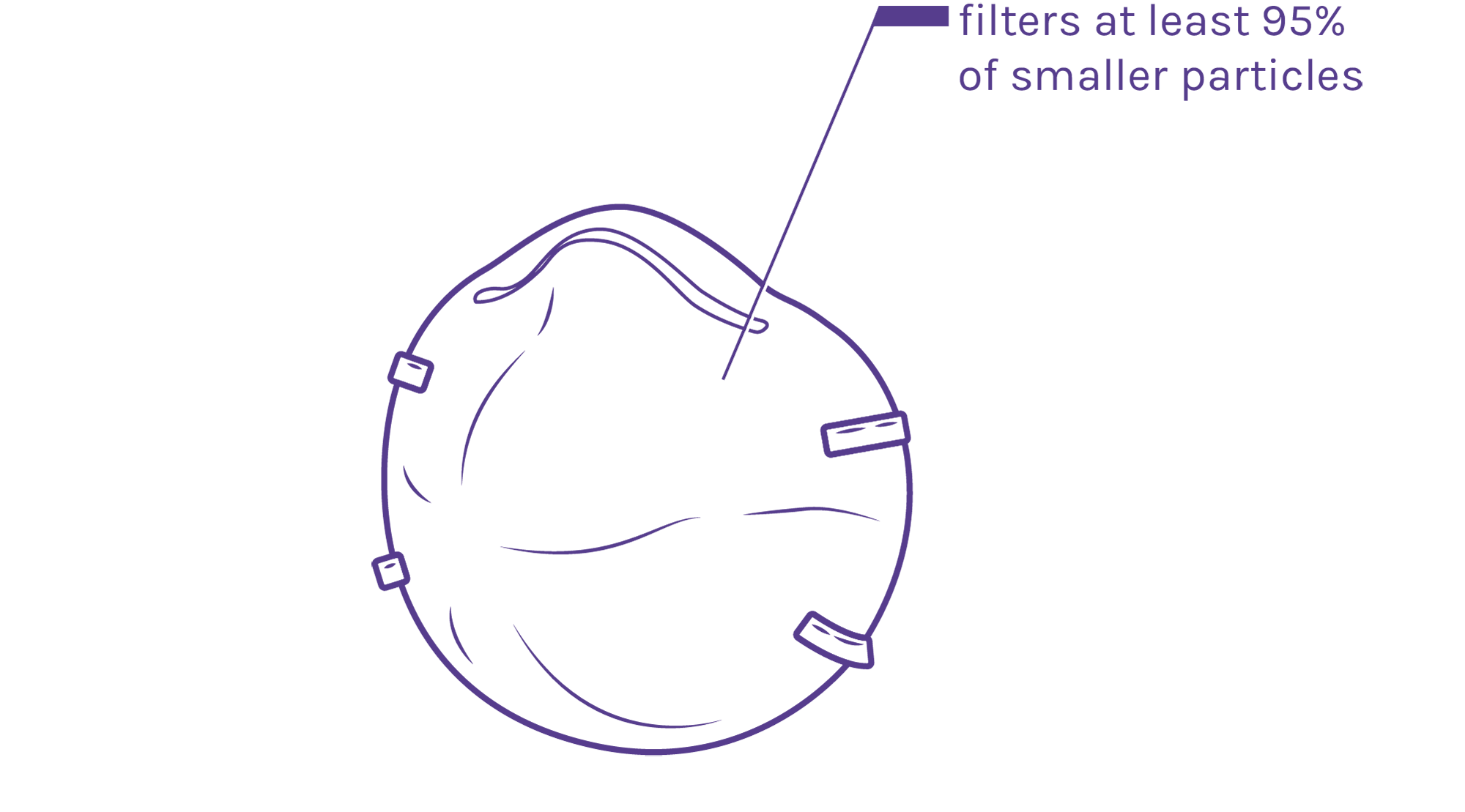
Will help prevent against catching and spreading COVID-19
If it has a breathing valve, does not effectively prevent the spread of COVID-19 if you are sick
For now, the CDC recommends only healthcare providers to wear surgical grade masks and N95 respirators, but this equipment is in short supply.
In order to maintain supply for the people who need it most, please do not hoard masks. If you do not already have surgical masks or respirators, do not buy them.
Instead, the CDC recommends the public to make their own cloth masks at home as an alternative to these masks to prevent the spread of germs.
Stay safe, stay well
Making your own mask to wear in public21
If you you need to go out in public, the CDC recommends wearing a cloth face covering which can be easily made with household items like t-shirts, bandanas, rubber bands, and coffee filters.


For instructions on how to make different variations of the masks, see the CDC's official instructions here.
When making these coverings, keep in mind that they must...
1. ...fit snugly but comfortably against the side of the face
2. ...be secured with ties or ear loops
3. ...include multiple layers of fabric
4. ...allow for breathing without restriction
5. ...be machine washable and dryable without damage or change to shape

For safety reasons, cloth face coverings should not be used by children under age 2, people with trouble breathing, or others that may not be able be able to take off the covering without assistance.
Make sure you wash these face coverings thoroughly and often after use, and that when you remove them from your face, you do not touch your eyes, mouth, or face with your hands.

Action Plan
How does the world respond to a pandemic?16
How does the world respond to a pandemic?16
A pandemic in the world is pretty scary. But the good news is that we have a plan on how to deal with situations like these.
World Health Organization (WHO)
Their primary role is to direct international health and provide global leadership and guidance on how to manage. Its headquarters are located in Geneva, Switzerland.
Each country has a Regional WHO Office
The US Regional Office is in in Washington, DC. Here, teams can communicate with the WHO headquarters and get up-to-date information about the emerging situation and consequently manage the outbreak response.
The WHO uses its international network of collaborating centers to collect information
In the US, the Centers for Disease and Control (CDC) in Atlanta, Georgia collects international and national data, analyzes that data, and synthesizes recommendations.
Our world is more connected than ever
This means that there are plenty of ways for diseases to spread to other people and places. There is a fine balance between protecting borders by quarantine and overreactions (that cause panic).
Local Emergency Operations Centers
Day-to-day operations are managed by a local ground team. These centers have a set of experts that work together to control the local situation.
Communications oversee how information is being disseminated to the public to ensure a strong unified voice.
Environment experts study the environmental causes related to the disease.
Epidemiologists analyze the distribution and patterns of the disease so that we can understand how it is affecting the population.
Incident Manager oversees the entire EOC, provides leadership to ensure coordination between the team, and is a liason to the regional office.
Policy makers ensure we have the regulations and permissions necessary to control the situation and may create new ones as needed.
Scientists analyze lab samples, research, and learn about the disease.
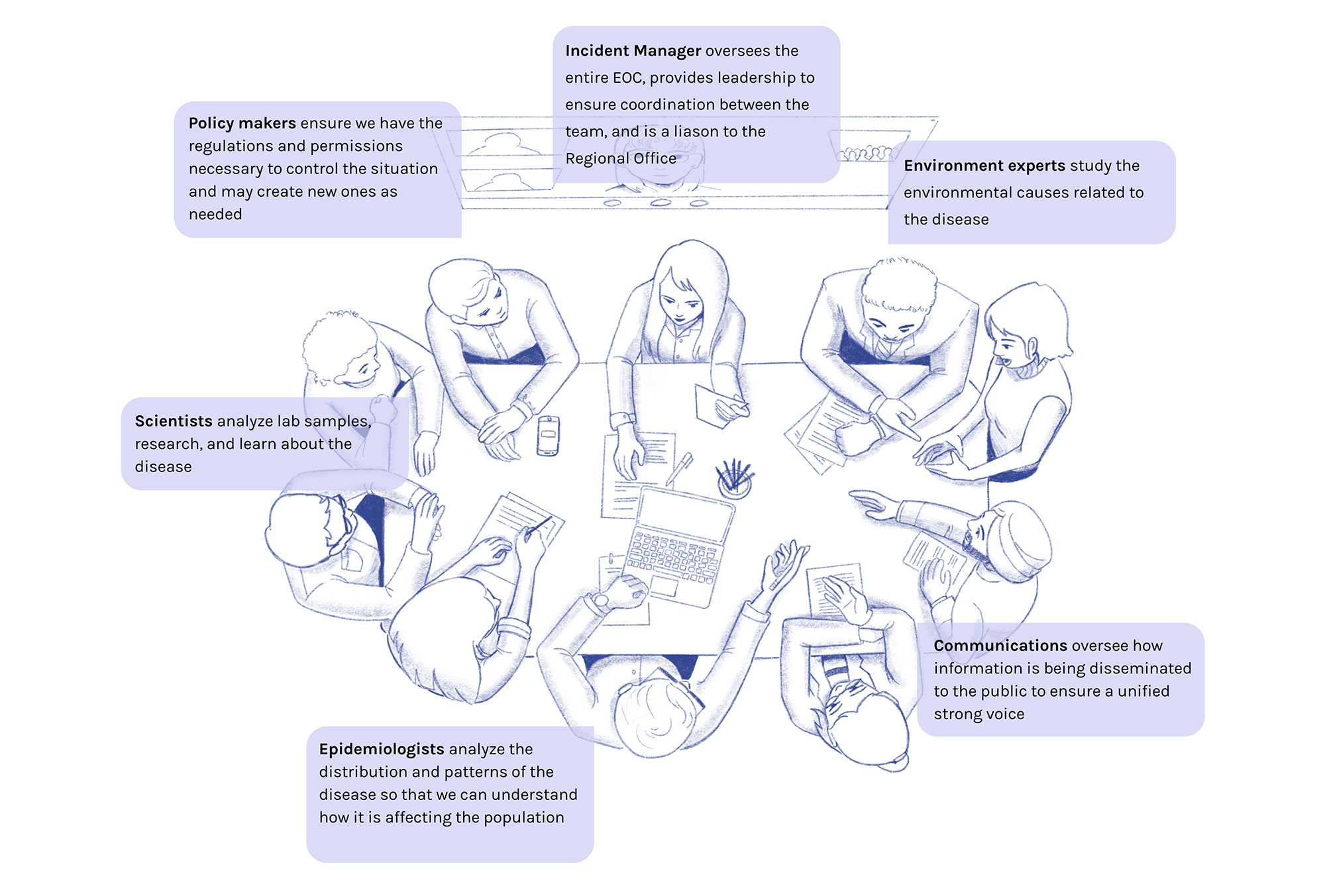
So what does this look like in practice?
So what does this look like in practice?
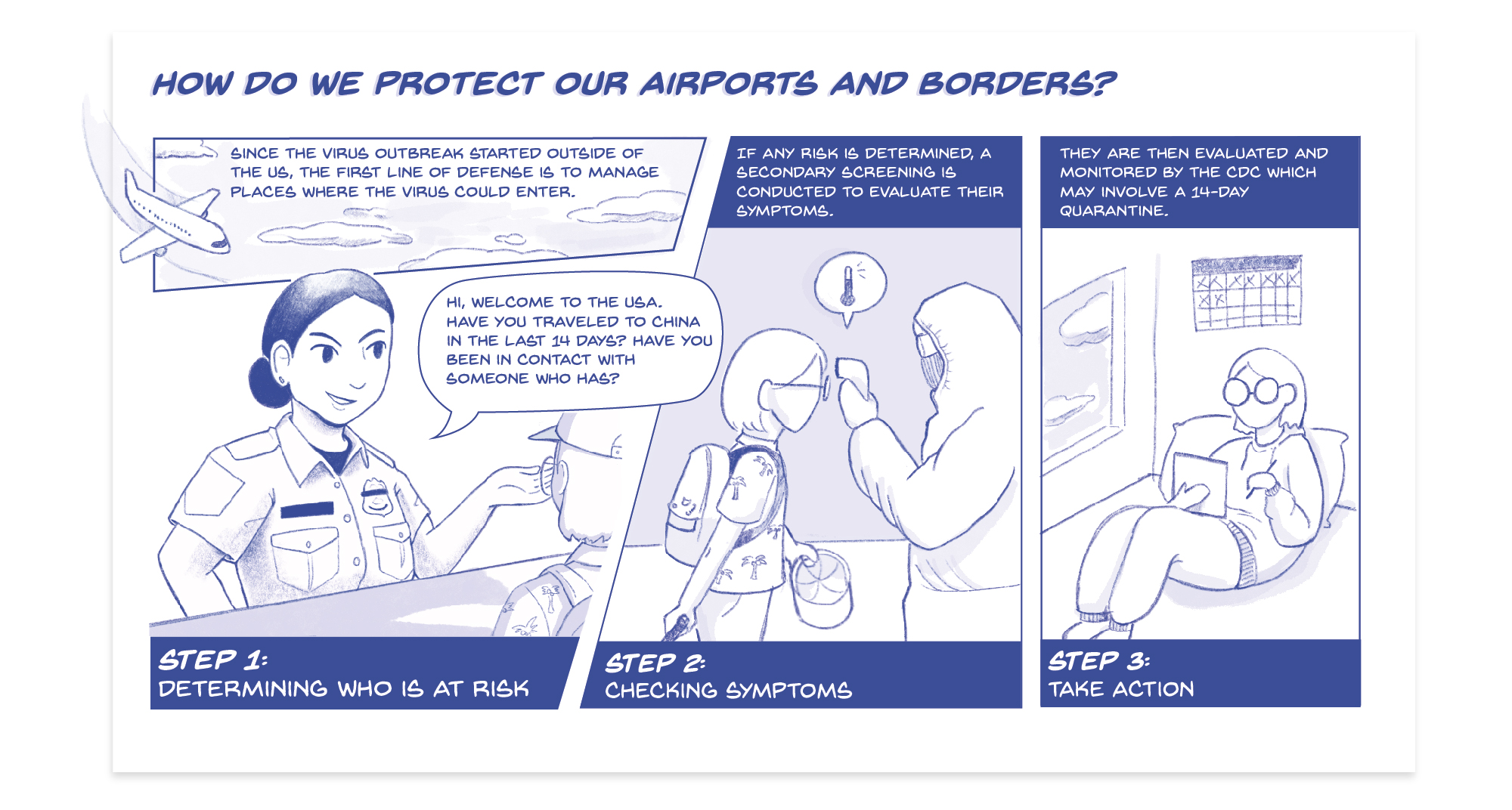
At the national level, our first line of defense is monitoring ports-of-entry11,14
Since the virus outbreak began outside of the US, the first line of defense is to manage places where the disease could enter. The CDC has ordered airlines to find out which passengers have traveled to China in the last 14 days and for major international airports to screen all incoming travelers.
The three-part process begins with Customs and Border Protection agents questioning travelers. Next, those at-risk are sent to a secondary screening by health workers where their temperature is taken. Then, those showing symptoms are evaluated and monitored by the CDC —which may involve a 14-day quarantine. Travelers who have been to China in the last 14 days are advised to stay home and monitor their symptoms.

If the virus enters a state, hospitals need to be prepared to respond2,12,15
If there is a suspected case of COVID-19 in the region, hospitals and local clinics should be trained in how to deal with the virus. Massachusetts General Hospital (MGH) is 1 of 10 CDC designated “regional ebola and special pathogen treatment centers” in the US —meaning that they have expert knowledge in how to deal with something like an outbreak. Many other hospitals have turned to MGH as they update their emergency plans.
If a city shuts down, what happens?10,7
In the US, it is very unlikely that the CDC would mandate an entire city be quarantined. US policy is actually to avoid location-based mass quarantines. Many experts have noted that the effectiveness of a mass quarantine for disease may not be worth the significant psychological and economic costs. However, in the case that a mass quarantine is ordered, cities have a plan to manage the situation.
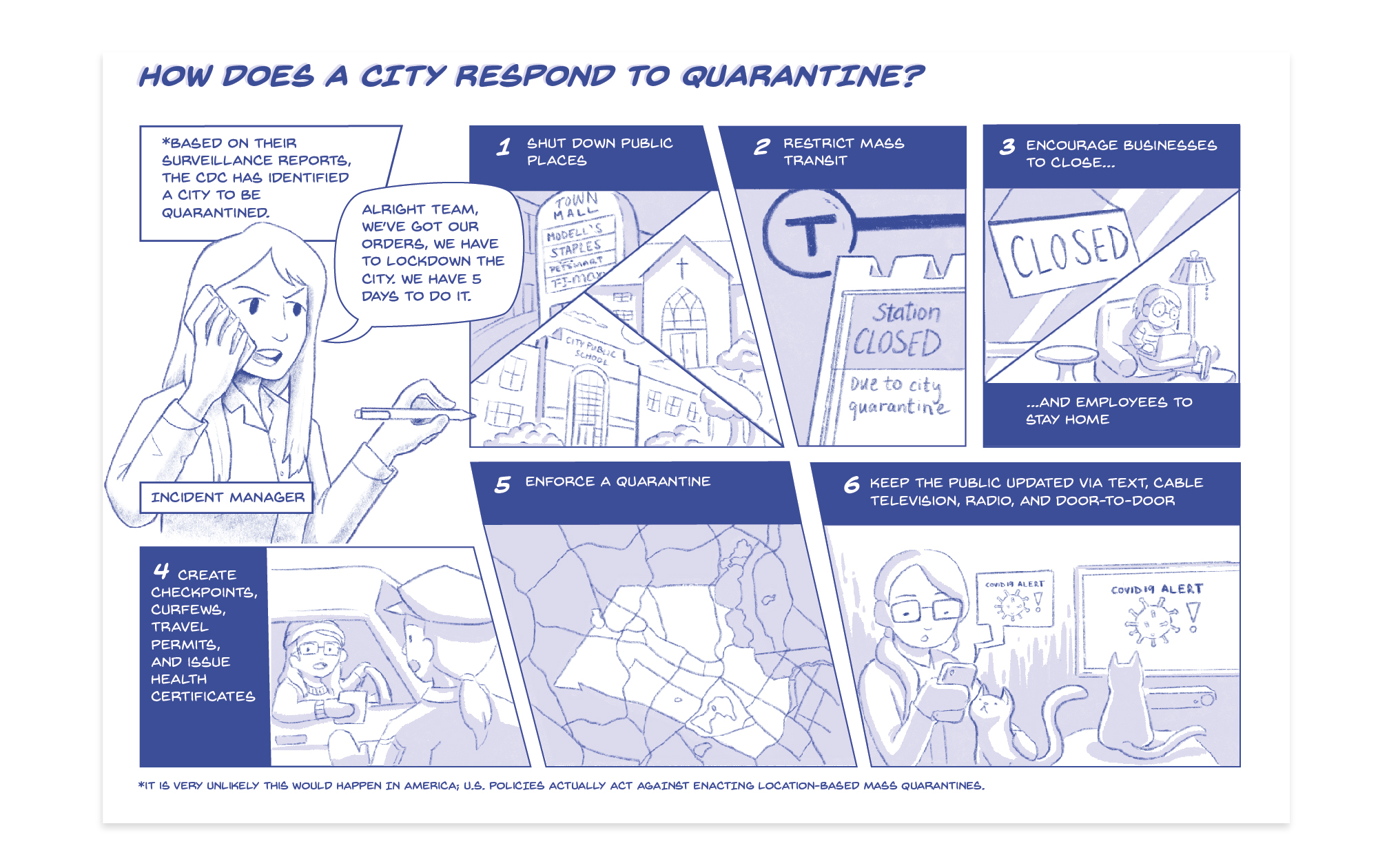


However, more extreme measures like this have not been required to deal with COVID-19 in the US.
For now, keep calm, follow regular flu season preventative measures, and keep up to date on the news for updates on protocols and treatment development.
While you may not see it, a lot of people are working to contain this virus so you can stay well.

Important Resources
World Health Organization
Information and guidance for the general publics.
Live update
https://www.who.int/emergencies/diseases/novel-coronavirus-2019
Centers for Disease Control and Prevention
Information and guidance for the general publics and healthcare professionals.
Live update
https://www.cdc.gov/coronavirus/2019-nCoV/
National Institute of Allergy and Infectious Diseases
https://www.niaid.nih.gov/diseases-conditions/coronaviruses
US Food and Drug Administration
https://www.fda.gov/emergency-preparedness-and-response/mcm-issues/novel-coronavirus-2019-ncov (archived link)

References
- Andrew, S. (2020, January 28). There's been a run of surgical masks in the US because of the coronavirus scare. You don't need them, physicians say. Retrieved January 28, 2020: https://www.cnn.com/2020/01/28/health/coronavirus-us-masks-prevention-trnd/index.html
- Bruce, M. (2020, January 31). 2019 Novel Coronavirus Response at the Brigham: 5 Things to Know: https://bwhbulletin.org/2020/01/30/2019-novel-coronavirus-response-at-the-brigham-5-things-to-know/
- Centers for Disease Control and Prevention. (2020, January 29). Prevention, Treatment of Novel Coronavirus (2019-nCoV). Retrieved February 5, 2020. (archived link): https://web.archive.org/web/20200205084838/https://www.cdc.gov/coronavirus/2019-ncov/about/prevention-treatment.html
- Centers for Disease Control and Prevention. (2020, January 28). What to do if you are sick with 2019 Novel Coronavirus (2019-nCoV). Retrieved January 31, 2020. (archived link): https://web.archive.org/web/20200131050853/https://www.cdc.gov/coronavirus/2019-ncov/about/steps-when-sick.html
- Centers for Disease Control and Prevention. (2020, January 29). Preventing 2019-nCoV from Spreading to Others. Retrieved January 31, 2020. (archived link): https://web.archive.org/web/20200131032657/https://www.cdc.gov/coronavirus/2019-ncov/hcp/guidance-prevent-spread.html#steps-for-caregivers
- Centers for Disease Control and Prevention. (2020, January 29). How 2019-nCoV Spreads. Retrieved February 6 2020. (archived link): https://web.archive.org/web/20200206092803/https://www.cdc.gov/coronavirus/2019-ncov/about/transmission.html
- Day, T., Park, A., Madras, N., Gumel, A., & Wu, J. (2006). When Is Quarantine a Useful Control Strategy for Emerging Infectious Diseases? American Journal of Epidemiology, 163(5), 479-485. doi: 10.1093/aje/kwj056
- Johns Hopkins CSSE. (2020 February 6). Coronavirus 2019-nCoV Global Cases by Johns Hopkins CSSE: https://gisanddata.maps.arcgis.com/apps/opsdashboard/index.html#/bda7594740fd40299423467b48e9ecf6
- Li, Q., Zhu, N., Munster, V. J., Phan, L. T., & Chinese Center for Disease Control and Prevention. (2020, January 24). Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus-Infected Pneumonia: NEJM. Retrieved January 31, 2020: http://www.nejm.org/doi/full/10.1056/NEJMoa2001316?query=featured_home
- New Hampshire CDC. State of New Hampshire Interim Severe Acute Respiratory Syndrome (SARS) Epidemic Preparedness Plan, (2004). (archived link): https://web.archive.org/web/20200306204414/https://www.dhhs.nh.gov/dphs/cdcs/sars/documents/sarsplan.pdf
- Pappas, S. (2020, February 4). Will airport screenings be enough to stop coronavirus in the US? Retrieved February 6, 2020.: https://www.livescience.com/can-airport-screening-stop-coronavirus.html
- Shenoy, E. (2020, January 24). Monitoring coronavirus. Retrieved February 1, 2020. (original source no longer available): https://www.massgeneral.org/news/hotline/HTL012420/monitoring-coronavirus
- Steinmetz, K. (2020, February 10). The U.S. Government Is Quarantining More Than 800 Americans. Here's Why That Very Rarely Happens. Retrieved February 11, 2020: https://time.com/5780049/coronavirus-quarantines-united-states/
- Tate, C. (2020, February 10). U.S. has screened 17,000 passengers for coronavirus at 11 airports since Sunday. Retrieved February 11, 2020: https://www.usatoday.com/story/travel/2020/02/07/coronavirus-u-s-passenger-screenings-11-airports/4693589002/
- Thielking, M., Loose, Y., Chu, J., Adam, Adsm, & Reach, J. (2020, February 7). U.S. hospitals call all hands on deck to brace for more coronavirus cases. Retrieved February 10, 2020: https://www.statnews.com/2020/02/07/hospitals-harnessing-resources-brace-spike-coronavirus-cases/
- World Health Organization. (2017). Emergency Response Framework (2nd ed.). Geneva. Licence: CC BY-NC-SA 3.0 IGO.
- World Health Organization. (2020, January 23). Middle East respiratory syndrome coronavirus (MERS-CoV). Retrieved January 31, 2020.: https://www.who.int/emergencies/mers-cov/en/
- Centers for Disease Control and Prevention. (2020, February 13). Coronavirus Disease 2019 (COVID-19) Situation Summary. Retrieved February 14, 2020. (archived link): https://web.archive.org/web/20200211031759/https://www.cdc.gov/coronavirus/2019-nCoV/summary.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcoronavirus%2F2019-ncov%2Fabout%2Fwhat-you-should-do.html#anchor_1580064337377
- The Novel Coronavirus Pneumonia Emergency Response Epidemiology Team. The Epidemiological Characteristics of an Outbreak of 2019 Novel Coronavirus Diseases (COVID-19) — China, 2020. China CDC Weekly, 2020, 2(8): 113-122.
- World Health Organization. (2020). Report of the Who-China Joint Mission on Coronavirus Disease 2019 (Covid-19) . Retrieved March 9, 2020: https://www.who.int/docs/default-source/coronaviruse/who-china-joint-mission-on-covid-19-final-report.pdf
- Centers for Disease and Control (2020, April 4). Use cloth face coverings to help slow the spread of COVID-19. Retrieved from (archived link): https://web.archive.org/web/20200404053838/https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/diy-cloth-face-coverings.html

Authors
Contributors

Special Thanks
Additional feedback provided by
Jan Benway
Grace Cordovano
Dorian Freeman
Eric Moreno
Joey Nichols, MD
Martin Pitt
Corinne Pritchard
James Rini, MD
Ernst-Jan van Woerden
Licensed under Creative Commons Attribution 4.0 license | Created by GoInvo
Send us Feedback | Check out the GitHub repo
Have feedback? Reach us at
coronavirus@goinvo.com









